Hearing test definition
A hearing test provides an evaluation of the sensitivity of a person’s sense of hearing and is most often performed by an audiologist using an audiometer. An audiometer is used to determine a person’s hearing sensitivity at different frequencies. The test will measure the quietest sound that can be heard several points across the speech range – this hearing test is termed an audiogram. Audiology evaluations consist of a series of tests used to determine whether a hearing loss exists and, if so, measure its type, degree and configuration. An audiologist will assess the results of each individual test in order to develop a treatment plan geared toward your unique hearing loss.
The hearing test will be performed by an audiologist, whether NHS or on a private basis the basics of the test should remain the same as described below. There are other hearing tests as well, e.g., Pure Tone Audiometry [PTA] test, Tympanometry test etc.
Getting the most from your appointment
At your appointment, you should be prepared to talk about all of the issues you have with your hearing (e.g. communicating, confidence, how you feel about your hearing) and whether you also experience any other problems associated with hearing loss (e.g. tinnitus). It’s important to talk openly about the different situations where you find it difficult to hear clearly (e.g. in noisy surroundings, in groups).
It might be useful to take someone else with you to this appointment. There is often a lot to remember and two heads are better than one!
Who Should Be Given an Audiology Evaluation?
An audiology (or hearing) evaluation can benefit patients of all ages, even those who do not exhibit signs of hearing loss.
Hearing loss is a progressive condition that often develops slowly. Many people are not aware of a change in their hearing because they gradually adapt to the subtle changes in their hearing ability over time. Studies indicate that it takes seven years, on average, for a hearing impaired individual to seek treatment.
An audiology evaluation should be the first course of action for anybody who even suspects a hearing loss. The sooner a diagnosis of hearing loss is made, the more successful treatment will be. Early detection means more options for the patient.
Many physicians urge making audiology evaluations a routine part of your overall health care, much like regular vision exams and dental checkups. They are quick, painless and provide immediate results.
What happens in a hearing test?
The audiologist performing your hearing test should introduce themselves and explain what is going to happen and the order of things to be done.
They will want to have a look into your ears to ensure there is no blockage (wax) or any reason the hearing test cannot be performed.
They will then want to take a brief history of your hearing, when you noticed problems, did they occur gradually or suddenly, have you had any infections or injury that may have caused the hearing difficulties and the problems you have had to deal with.
The audiologist will then want to test your hearing by performing an audiogram. The test will take about 20-30 minutes. You will be played a series of sounds through headphones and be asked to respond in some way that you have heard the sound normally by pressing a button every time no matter how quiet or faint.
This is done in one ear and then the other, as the results can be different. Depending on the result there may be other tests required, but this will be explained at the time.
Your hearing test results
Sound is measured in two key ways:
- volume or level – measured in decibels (dB)
- pitch or frequency (whether it’s high or low) – measured in hertz (Hz)
Your audiologist will probably refer to these two things when they explain the results of your test to you. If you do want to a copy of the test, it’s best to ask on the day.
What Does Diagnostic Testing Entail?
A comprehensive audiology evaluation consists of a series of individual diagnostic tests that measure different aspects of your hearing. Following a physical examination and a review of your medical history, you will be given any or all of the following tests:
Pure Tone Testing
Pure-tone testing (also known as pure tone audiometry) uses air conduction to measure your ability to hear sounds of various pitches and volumes. Wearing headphones, you will be asked to identify a series of tones by raising a hand, pressing a button, or responding verbally.
The results are charted on an audiogram, a graph that shows the type, degree and configuration of your hearing loss by comparing pitch (frequency) with loudness (intensity). The pattern recorded will help your audiologist determine your hearing threshold.
Bone Conduction Testing
Bone conduction testing is another type of pure-tone test that measures the inner ear’s response to sound. If there is damage or a blockage in the outer or middle ear, bone conduction audiometry testing may be used.
Instead of sending the tones through the ear, this type of testing is able to bypass the outer and middle ear and send the tone directly to the inner ear. A small vibrator is placed behind the ear. The device sends out a vibration that passes through the skull bone to reach the inner ear.
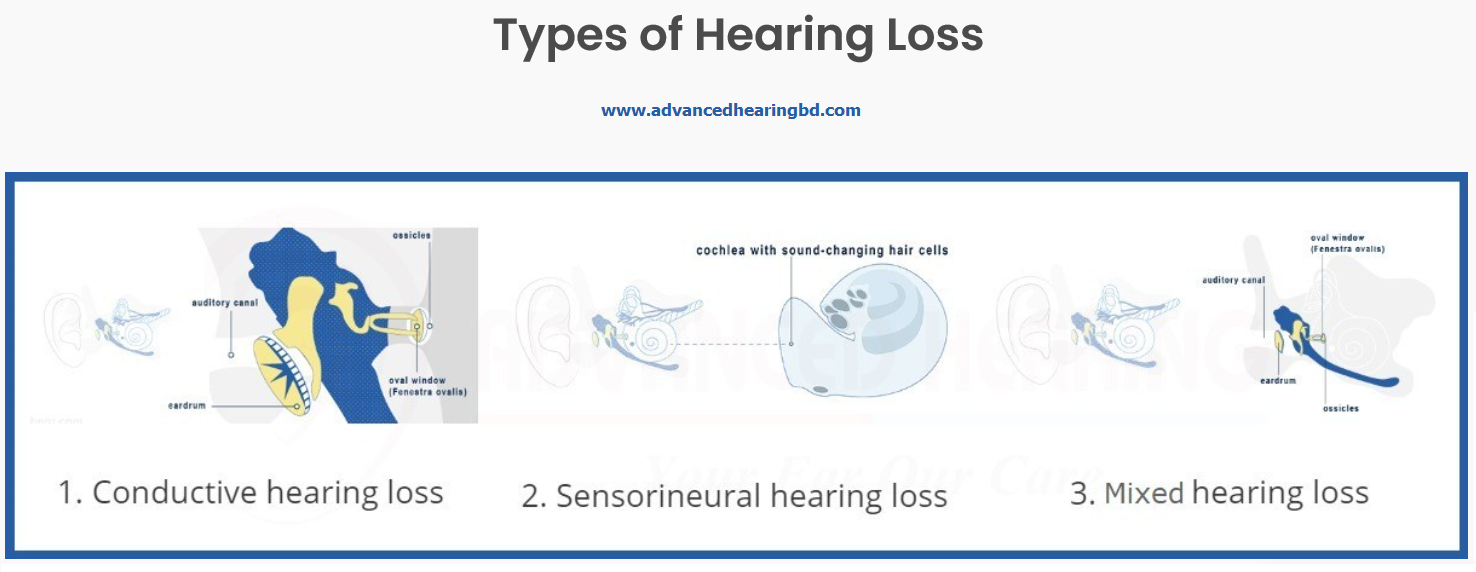
If the results of this test are different than the air conduction test, your audiologist can use this information to determine whether you have a conductive or sensorineural hearing loss.
Alternatively, a two-pronged metal tuning fork may be placed behind the ear or on the forehead. When vibrated, it produces a tone that travels to the cochlea via the skull. Your response determines how well sound travels through different parts of your ear, helping the audiologist diagnose your type of hearing loss.
Bone conduction testing is often used in place of air conduction testing when an obstruction in the outer or middle ears is present.
Speech Testing
Speech (or word recognition) testing is used to measure your speech reception threshold (SRT), or the faintest speech you can understand 50 percent of the time. This is compared with your pure-tone test results to confirm the diagnosis. In addition, your ability to separate speech from background noise will be recorded.
Speech testing may be administered in either a quiet or noisy environment; results are recorded on the audiogram for easy visual reference.
Tympanometry
Tympanometry is a test of the middle ear used to detect fluid, wax buildup, eardrum perforations and tumors. It measures movement of the eardrum in response to air pressure; the results are recorded on a chart called a tympanogram.
Acoustic Reflex Testing
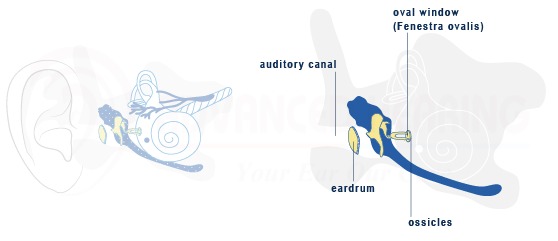
The acoustic reflex test measures involuntary muscle contractions of the middle ear, and is used to determine the location of your hearing problem (the ossicles, cochlea, auditory nerve, etc.) as well as the type of hearing loss.
Auditory Brainstem Response (ABR)
Auditory brainstem response testing is used to determine whether a specific type of hearing loss – sensorineural – exists. It is also frequently used to screen newborns for hearing problems.
In an ABR test, electrodes are attached to your head, scalp or earlobes, and you are given headphones to wear. Your brainwave activity is measured in response to sounds of varying intensities.
Otoacoustic Emissions (OAEs)
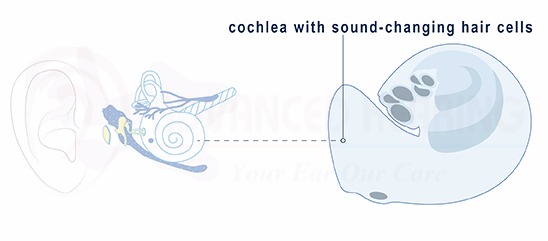
Otoacoustic emissions (OAEs) are sounds generated by vibrations of the hair cells in the cochlea of the inner ear. OAE testing utilizes a tiny probe fitted with a microphone and speaker that is used to stimulate the cochlea and measure its response. Individuals with normal hearing will produce emissions; when a hearing loss exceeds 25-30 decibels, no sound will be produced.
This test helps determine whether there is a blockage in the ear canal, excess fluid in the middle ear or damage to the hair cells of the cochlea. OAE testing is often included in newborn hearing screening programs.
Audiograms
Hearing tests are usually carried out in a quiet environment which is sound damped from external noise. The person whose hearing is being tested listens to sounds transmitted by an audiologist and presses a button to signal when they have heard something. The results of the test are plotted on an audiogram.
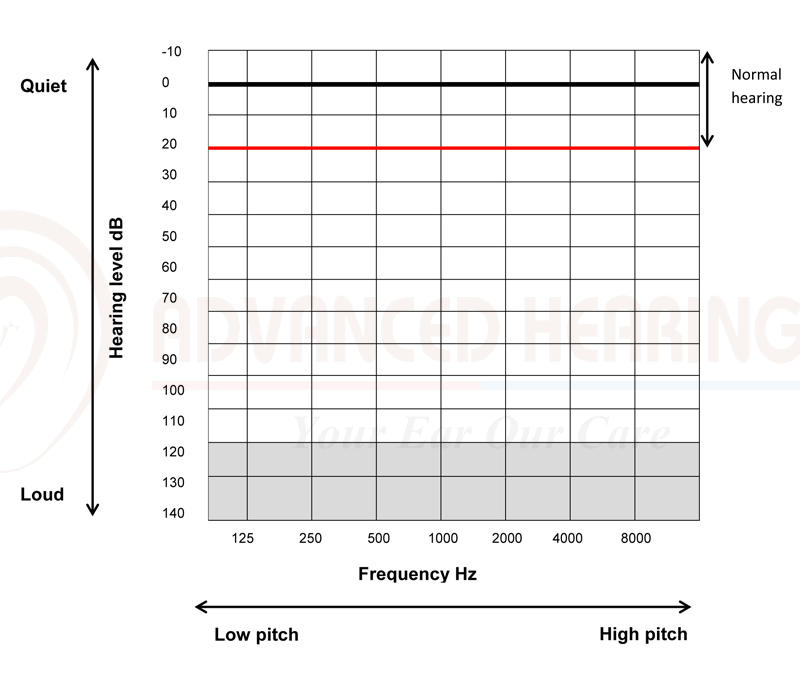
Volume or loudness which is measured in decibels (dB). Sounds become louder from the top down – softest near the top of the graph.
Pitch or frequency which is measured in hertz (Hz). Frequency goes from low (125Hz) on the left to high (8000Hz) on the right – similar to a piano (low notes on the left, higher to the right).
Normal hearing is when the softest sounds heard are between -10 and 20 dB. If the sounds are louder than 20 dB and you still can’t hear them, then there is a hearing loss. The further down the chart the line of your hearing test comes, the more of a hearing loss.
Mild hearing loss is between 21dB and 40dB. You often have difficulty following speech especially in noisy situations. This type of loss is often noticed by family first rather than yourself.
Moderate hearing loss is between 41dB and 70dB. You often have difficulty following speech and other quiet noises.
Severe hearing loss is between 71dB – 90dB. You are unable to hear speech even in quiet surroundings and do not hear general noises such as traffic unless it’s loud.
Profound hearing loss is greater than 90dB. You are unable to hear most sounds unless really loud.
Thresholds
In the audiology clinic, testing is done with headphones; we call them ‘air conduction thresholds’ as the sound must travel through the air of the ear canal to be heard. This process allows the audiologist to test the full hearing system.
Alternatively, hearing can be tested using a bone conductor – a device that rests on the bone behind the ear (held in place by a metal band stretching over the top of the head). This bone conductor transmits sound vibrations through the bones of the skull directly to the inner ear. This process allows the audiologist to test the hearing of the inner ear directly.
The audiologist would compare the air conduction and bone conduction results to determine where any hearing loss occurs.
The threshold of hearing at any tone/frequency is the quietest sound heard – this is what is recorded on the audiogram for each ear air conduction and bone conduction.
Speech banana
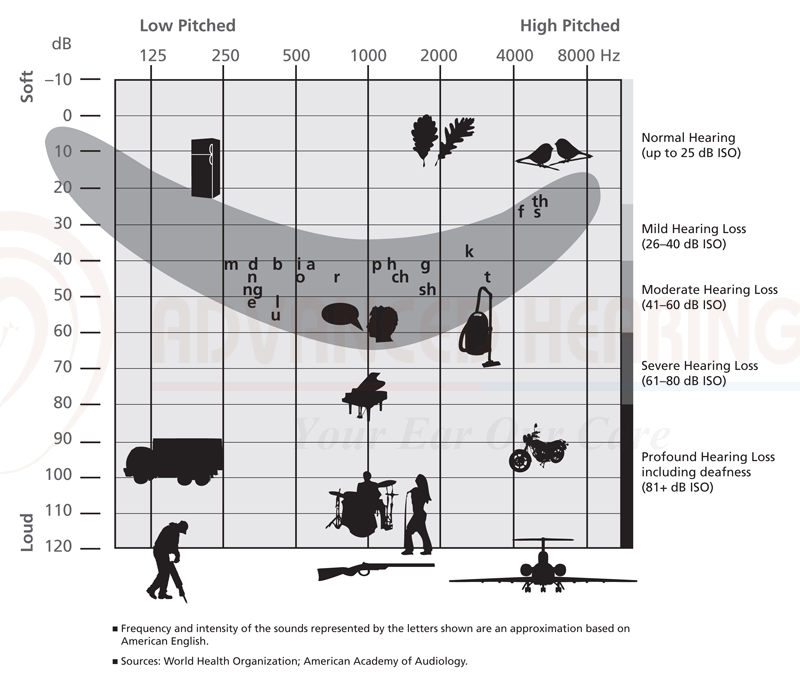
A useful way to look at the audiogram chart is with a ‘speech banana’ superimposed on it. The speech banana is so called because of its shape. It represents the level/intensity and tone/frequency of sounds of speech in language, which when placed on the audiogram, forms a banana like shape.
The chart below shows a speech banana superimposed on an audiogram chart with the different letters of speech and also where other common noise occurs.
Speech audiogram testing
Most audiologists will now also perform a ‘speech audiogram’ to see how well you hear speech. This will normally involve getting you to listen to speech (either single words or very short sentences) through headphones or a loud speaker, and asking you to repeat exactly what you have heard.
This can be done in the presence of background noise or in quiet surroundings depending upon the test procedure used.
This test gives the audiologist information as to what can be achieved with amplification and what level of improvement could be made to your hearing.
Screen your own hearing
There are several ways to check your own hearing from the comfort of your own home.
Whilst these screening tests are useful, they should not be taken as a diagnostic test of your hearing and if in any doubt to discuss the results with your GP or local audiologist.
Online screening hearing tests are available from the majority of hearing aid manufacturers and major suppliers or dispensers. They can be found by typing ‘Online hearing test’ into search screens.
Advanced Hearing Center Audiological Services
Pure Tone Audiometry [PTA]
Description :
It assesses the Frequency Specific Hearing Sensitivity Level (upto 8 kHz) subjectively.
Validation of Report: Around 3 months (depends on advancing age & Pathological conditions).
Eligibility Criteria:
- Intact/Normal intellectual Functioning level.
- Age range is around > 6 years.
Immittance Audiometry (Low Frequency Tympanometry & Acoustic Reflexometry)
Description:
It is objectively assesses mobility of the Tympano-Ossicular system as well as to rule out any Middle Ear Pathology (Tympanometry) & assesses the Acoustic Reflex Pathways (Ipsi & Contra) (Acoustic Reflexometry).
Test Preparation:
Chewing, Swallowing, & Head or body movements are not allowed during testing as well as during sedated deep sleep, positive pressure may build up in the Middle Ears, which can compromise the results; although positive Middle Ear Pressure does not have any significant diagnostic values.
Validation of Report:
Around 3 months (depends on advancing age & Pathological conditions).
Eligibility Criteria:
Patient having Active Otorrhea, Severe Otalgia, H/O recently operated Ear(s), Impacted Cerumen/Debris in EAC, Anatomical Deformities (Aural Atresia/Stenosis), Perilymphatic Fistulas are generally not a reliable candidate for tympanometry & Tullio Phenomenon and Hyperacusis suffering patients for Acoustic Reflexometry .
Speech Audiometry [SRT+SDS]
Description:
Speech Audiometry (SRT, SDS/WRS, SAT, MCL, UCL, DR, Rollover Ratio or PI-PB Function etc.)
is subjectively assesses the speech perception ability of the patient & Rollover Ratio is used to rule out Cochlear from Retrocochlear Pathology.
Validation of Report:
Around 3 months (depends on advancing age & Pathological conditions)
Eligibility Criteria:
- Intact/Normal intellectual Functioning level.
- Age range is around > 8 years.
- Typical Sensory/Neural Hearing Loss is required otherwise outcome will be Insignificant for Rollover Ratio.
Tone Decay Test [T.D.T]
Description:
Tone decay test is used to rule out Cochlear from Retrocochlear Pathology subjectively.
Validation of Report:
Around 3 months (depends on advancing age & Pathological conditions).
Eligibility Criteria:
- Intact/Normal intellectual Functioning level.
- Age range (generally > 8 years) is depends on Intellectual Functioning Level of the Patient.
- Typical Sensory/Neural Hearing Loss is required otherwise outcome will be Insignificant.
- For Alternate Binaural Loudness Balance Test & Supra Threshold Adaptation Test, Unilateral or Asymmetrical Sensory/Neural Hearing Loss (>40 dB or more) is required.
Short Increment Sensitivity Index [S.I.S.I]
Description:
SISI test is used to rule out Cochlear from Retrocochlear Pathology subjectively
Validation of Report:
Around 3 months (depends on advancing age & Pathological conditions)
Eligibility Criteria:
- Intact/Normal intellectual Functioning level.
- Age range (generally > 8 years) is depends on Intellectual Functioning Level of the Patient.
- Typical Sensory/Neural Hearing Loss is required otherwise outcome will be Insignificant.
- For Alternate Binaural Loudness Balance Test & Supra Threshold Adaptation Test, Unilateral or Asymmetrical Sensory/Neural Hearing Loss (>40 dB or more) is required.
Tinnitus Matching / Masking
Description:
It is used for (audiological) assessment & management of tinnitus subjectively.
Test Preparation:
Pure Tone Audiometry is mandatory before this.
Validation of Report:
Around 1 month (depends on advancing age Pathological conditions).
Eligibility Criteria:
- Intact/Normal intellectual Functioning level.
- Age range is generally adult population.
Tinnitus Retraining Therapy [T.R.T]/Per Sitting
Description:
TRT is a threapy for reducing tinnitus in ear. This therapy is done when patient having tinnitus (ringing sound) in ear. You have to sit idle when threapy is don. Tinnitus Matching result are used to do Tinnitus Threapy. Audiometer is used for tinnitus therapy. It requires several sitting (vary from patient to patient) to reduce tinnitus. No preparation required for this test.
Test Preparation:
Report considered to be valid till 3 to 6 months if other wise no significant changes taken place.
Eligibility Criteria:
If Tinnitus Matching is done then only therapy continues otherwise these therapy not done. Drunken & drug addicted people or people suffering from contaminated diseases are not allowed for this test.
B.E.R.A / A.B.R. [ Brainstem Evoked Response Audiometry ] Diagnostic
Description:
Auditory Brainstem Response (ABR)/ Brainstem Evoked Response Audiometry (BERA) [Diagnostic]
Air Conduction ABR:
It is used for Site of Lesion (differentiate Cochlear from Retrocochlear Pathology) testing & for threshold estimation (average degree of Hearing Level) objectively; in difficult to test population.
Bone Conduction ABR:
It is used to detect Average Bone Conduction Hearing Level as well as Type of Hearing Loss, objectively (only in combination with Air Conduction ABR) & in presence of Anatomical Deformities like Aural Atresia/Stenosis etc.
Test Preparation:
Sedation or Natural sleep is generally required for elimination of Muscle Artifacts.
Validation of Report:
Around 3 months (depends on advancing age & Pathological
Conditions)
Eligibility Criteria:
- Age range is generally > 3 months.
- Patient having Active Otorrhea, Impacted Cerumen/Debris in EAC, Anatomical Deformities (Aural Atresia/Stenosis), are generally not a candidate for this test.
A.S.S.R [Auditory Steady State Response]
Description:
Auditory Steady State Response/ASSR Or Amplitude Modulation Following Response/AMFR or The Envelop Following Response/EFR or Steady State Evoked Response/SSER or Steady State Evoked Potential/SSEP [Diagnostic]
It assesses Frequency Specific (500 Hz to 4 kHz) average Hearing Sensitivity Level (degree of Hearing) objectively in difficult to test population.
Test Preparation:
Sedation or Natural sleep is generally required for elimination of Muscle Artifacts.
Validation of Report:
Around 3 months (depends on advancing age & Pathological
Conditions).
Eligibility Criteria:
- Age range is generally > 2 months.
- Patient having Active Otorrhea, Impacted Cerumen/Debris in EAC, Anatomical Deformities (Aural Atresia/Stenosis), are generally not a candidate for this test.
Oto Acoustic Emission Test [O.A.E] Diagnostic
Description:
Oto Acoustic Emissions/OAEs (Distortion Product & Transient Evoked) [Diagnostic]
It assesses the Outer Hair Cells Functioning upto Periphery Level & to rule out Auditory Neuropathy Spectrum Disorders, objectively (only in Combination with Air Conduction ABR).
Test Preparation:
Sedation or Natural sleep is generally preferred but in awake condition with quiet state, this test is done successfully.
Validation of Report:
Around 3 months (depends on advancing age & Pathological Conditions).
Eligibility Criteria:
- Age range is generally > 24 hours after birth.
- Patient having Active Otorrhea, Impacted Cerumen/Debris in EAC, Anatomical Deformities (Aural Atresia/Stenosis), are generally not a candidate for this test.
Find Best Hearing or Audiological test in Bangladesh! Call us at +8801755574799 to schedule a free hearing consultation, or find your nearest clinic to book an appointment online.